Multiple Specialities,
Singular Focus
Discover the wide range of specialities that our hospital Dubai focuses on. We pride ourselves on coupling the latest advances in medical technology with a hand picked team of medical experts, doctors and surgeons.
THE FUTURE OF HEALTHCARE, TODAY
Take a virtual tour of Valiant Clinic & Hospital Dubai and learn more about the dedicated handpicked team of specialists, doctors and surgeons ready to help patients with world class standards and healthcare facilities in the Middle East dedicated to patient comfort and well being.
PARTNERING WITH LEADING MEDICAL INSURANCE PROVIDERS
As a Dubai Hospital with a board certified handpicked team of world class experts dedicated to patient comfort, we work with leading medical insurance providers in the country, if you have any questions or queries just give us a call on 8008254268.

hospital dubai

Dubai Hospital

Dr Dubai Hospital

Dr Hospital Dubai UAE

Hospital Dubai

Hospital Dubai

Specialist Hospitals Dr Doctors




DHA Hospital Dubai

Dubai Hospital

Hospital in Dubai

MEET OUR HANDPICKED TEAM OF EXPERTS
- All
- Anesthesiology
- Aviation Medicine
- Bariatric Surgery
- Brain Surgery
- Cardiac Surgery
- Cardiology
- Diet and Nutrition
- Electrophysiology
- Endocrinology
- ENT
- Family Medicine
- General Surgery
- Gynecology
- Hip Surgery
- Internal Medicine
- Knee Surgery
- Laparoscopic Surgery
- Nephrology
- Neurology
- Neurosurgery
- Obstetrics
- Optometry
- Orthopedic
- Plastic Surgery
- Psychology
- Rhinoplasty
- Spine Surgery
- Urology

A HOSPITAL IN DUBAI DEDICATED TO YOUR HEALTH & WELLBEING
Valiant Clinic & Hospital provides a comprehensive range of medical services and specialties that cater to the health and overall wellness of an individual, as well as the larger community.
We are focused on leveraging the latest advances in modern medical technology to bring direct benefit to our community by adopting a patient-centric approach at our hospital in Dubai. As a vibrant and innovative city, Dubai offers our patients a wide range of options for high quality medical healthcare, and each day is a new opportunity to advance our goal of ensuring we remain their choice as the best hospital in Dubai.
With dedicated inpatient and outpatient facilities that are well equipped and staffed by a handpicked team of specialists, doctors and surgeons, we are able to assist with a wide variety of patient care that ranges from surgery for less complicated outpatient procedures to more complicated inpatient procedures which we can cater for via our rooms and VIP inpatient rooms.
LEADING CARDIOLOGY EXPERTS WITH ADVANCED MEDICAL TECHNOLOGY
Our specialist team of cardiologists in Dubai have clinical expertise and a dedication to excellence in the treatment of cardiovascular diseases and conditions. At our hospital in Dubai we have invested heavily in exploiting the latest advances in medical technology at hand to help in diagnosis and treatment.
Our cath lab and clinical suite includes the highly advanced Philips Azurion C12 with advanced 12″ flat detector and a Carto ® 3 System, which features advanced imaging technology that allows diagnosing physicians to gain insights using the latest developments in electromagnetic technology to build real-time three dimensional (3d) maps of a patient’s cardiac structures.

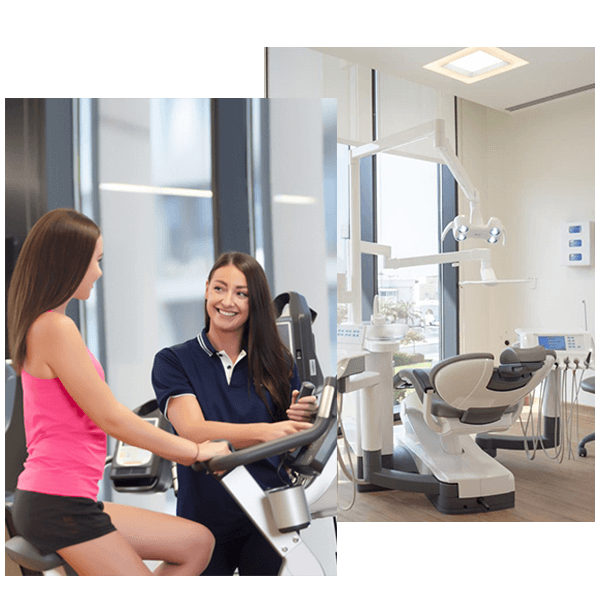
WORLD CLASS EXPERTS IN JOINT REPLACEMENT AND DUBAI SPORTS MEDICINE
Our orthopedic surgeons in Dubai are experts in joint replacement including knee replacement and hip replacement. Complementing our state of the art medical treatments is our focus on sports medicine. Our sports medicine team is focused on delivering the highest standards of care to a broad spectrum of patients that range from fitness enthusiasts to professional athletes.
One of the benefits of being a multispeciality hospital is the immediate availability of a wealth of knowledge that spans multiple medical disciplines. Dedicated facilities that range from the latest in robotic medical innovation to high resolution imaging and resonance scanners means we have the tools to make the correct diagnosis in a timely fashion, shortening the treatment and recovering period. Our health packages and healthcare facilities are world class, dedicated to patient comfort and providing the ultimate standards for patient comfort in the Middle East.